PeriodontiumThe periodontium consists of the tissues that support the teeth. It includes:
|
 The periodontium must be healthy during an orthodontic treatment. The arrow indicates an area of gum recession where a part of the root is uncovered. (ill. Colgate) |
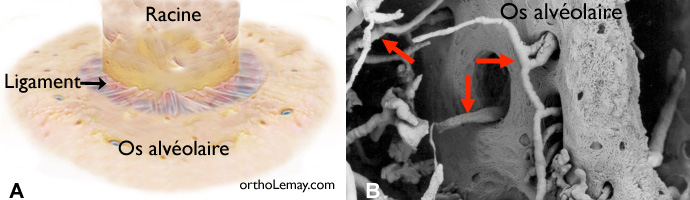
The periodontal ligament is a very important structure in orthodontic tooth movement and the stability of teeth in general. (A) It contains fibers that attach the tooth root to the alveolar bone that surrounds it. The ligament space between the tooth and the root (0.25 mm) allows light tooth movement when a force or pressure is applied to the teeth (chewing, teeth clenching, etc.). (B) Small blood vessels (capillaries) irrigate and nourish the bone and ligament. Specialized cells will remove bone from certain areas and will deposit some in other areas, which makes it possible to move teeth orthodontically on distances in the order of several millimeters. ((B) Capillaries of the periodontal ligament of a young rabbit – Kronka 2001)
- Orthodontically, the periodontium is of crucial importance since it must be healthy, intact and of the best quality possible to allow multiple tooth movements throughout an orthodontic treatment.
- Its structures are fragile and can be easily damaged if inadequate forces are applied. Moreover, bad oral hygiene may damage or destroy its components and make normal tooth movements impossible.
- The quality of the periodontium may vary from one person to another and its evaluation includes the quality and quantity of tissues present. Heredity plays a significant role in determining a person’s type of tissues.
- The gum is formed by a keratinized epithelial tissue and collagenous fibers that attach the gingiva to the alveolar bone and to the cementum of the tooth (attached gingiva). This makes the gum resistant to masticatory constraints.
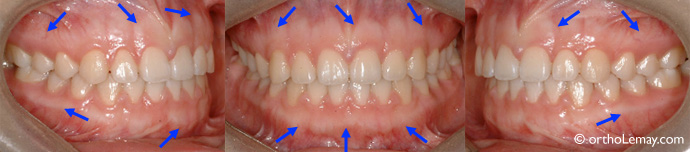
The quality of this 17-year-old girl’s gingiva is excellent. The arrows indicate the extent of the protective keratinized gingiva. Gingival recession affects this protective tissue band and makes teeth more vulnerable. If the gingival recession is significant, surgical procedures can try to restore the affected tissues.
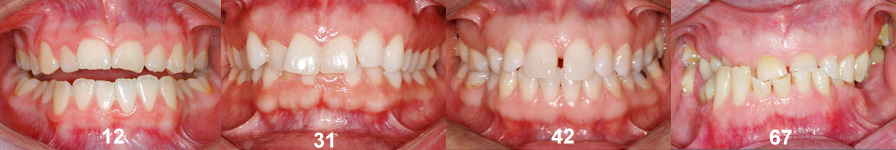
It is possible to have a normal periodontium at any age, even with a significant malocclusion. All these people have an ideal periodontium; a good quantity and quality of gum and bone protect and support the teeth, regardless of their age (indicated on the pictures). Such tissues are excellent to envision orthodontic corrections since they will adequately support the teeth when they move.
Gingival recession (receding gums)
Recession – Gingival problems
Gingival recession, also known as receding gums, is a condition that appears as a decrease in the level of gingiva and bone around one or several teeth, which exposes the tooth root.
- The gum around the teeth plays a protective role by creating a type of sealing around them.
- When the quantity of gum covering the teeth decreases significantly (severe recession), this can jeopardize their health and survival.
- Gingival problems mostly affect adults, but they may occur at any age.
- This process can be progressive and can expose the surface of the root as time goes by.
The most common causes of gingival loss include:
- Chronic infection of dental tissues,
- abrasion by an inadequate brushing technique or a technique that is too aggressive,
- traumatic wear caused by other teeth biting on the gingiva,
- malocclusion: a significant malposition of teeth, such as when a tooth is outside the dental arch or severely rotated (see example – picture),
- gingival wear caused by a “piercing“.
Does orthodontics cause gingival recession?
- When certain conditions are met during an orthodontic treatment, recession may appear or worsen when teeth are moved. This usually affects the anterior lower teeth, but can affect any tooth.
- To learn more on the subject and see other examples.
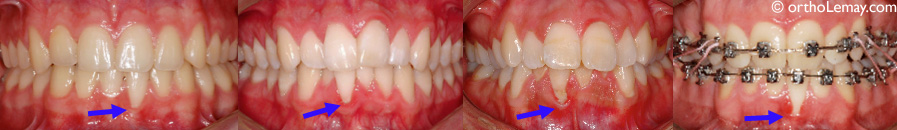
A few examples of receding gums affecting lower incisors. The most severe cases are referred to a general dentist or periodontist to evaluate the need to perform a gingival graft or another mucogingival procedure.
Malocclusion and periodontium integrity
- Certain malocclusions can directly contribute to damaging the periodontium when teeth are in contact with the gum or the palatal mucosa.
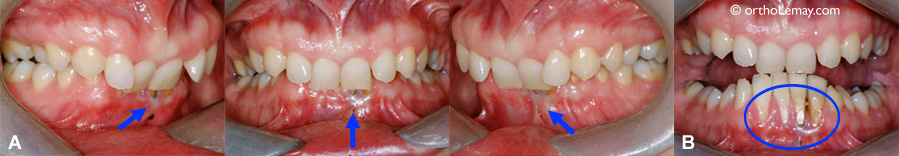
The Class II division 2 malocclusions can particularly be destructive for the front part of lower incisors and the gum that covers them. (A) Closed mouth. (B) When the mouth is open, the significant tooth wear (crowns and roots) and gum wear can be seen in this 37-year-old woman. The gingival recession is caused by the excessive overbite between the upper and lower incisors.
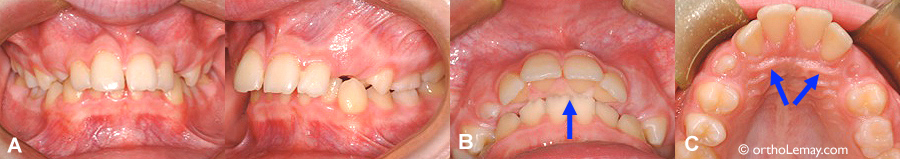
Class II malocclusions with a significant overjet (division 1) often come with an excessive overbite, causing the inferior incisors to bite into the palatal mucosa. (A) This kind of problem can appear very early, as in this 11-year-old young patient who shows an 11-mm gap between the anterior teeth. (B) An upper occlusal view shows the lower incisors that bite into the palate. (C) The marks left by the lower incisors are visible on the surface of the mucosa. If this condition is not corrected, the periodontium can continue to progressively deteriorate throughout the years and significant gingival recession and bone loss may result, up to jeopardizing the solidity of teeth.
- An extreme malposition of a tooth in the dental arch may cause not only receding gums, but also the loss of some of the alveolar bone that supports the tooth. Correcting this malposition orthodontically may improve this condition, but does not always make it possible to restore the missing tissues (bone and gum).
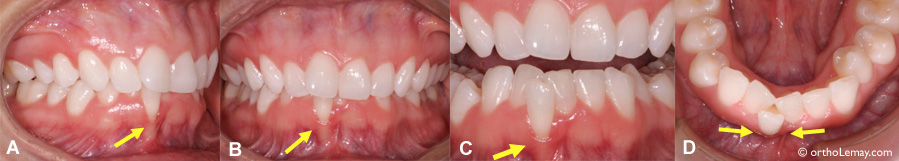
This 29-year-old woman suffers from a significant gingival recession, as well as bone loss, in front of a lower incisor (A and B). This is obvious when the level of gingiva is compared to the normal level present around the adjacent teeth. (C and D) When the mouth is open, it is easy to see that the main cause of this loss of tissues is the significant lack of space that “forces” the incisor to move forward in a position that is outside the arch.
Gingival graftingWhen the loss of tissues is significant and can jeopardize the long-term survival of one or several teeth, it may be indicated to correct the missing gum using a “gingival graft“. This term refers to different periodontal surgical procedures aiming at covering the denuded roots with oral tissues.
|
 |
Indications
The main objectives of gum grafts are to:
- Prevent additional gingival loss on the roots affected by recession.
- Increase the quantity of gum to stop the progression of the recession.
- Decrease or eliminate the sensitivity of recessed roots.
- Improve esthetics by covering the visible roots.
- Decrease the susceptibility to caries that could affect the roots.
To read the testimonial of a patient who underwent a gingival graft.
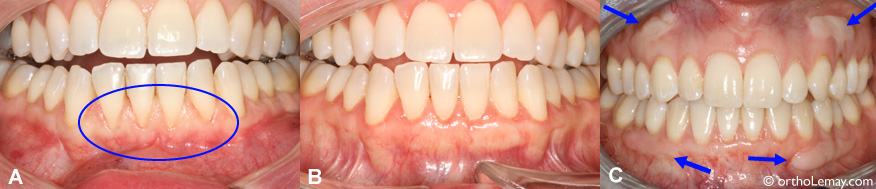
(A) Moderate gum recession affecting the lower incisors. (B) After a connective tissue graft, the quantity and appearance of the gum are normal and the graft can practically go unnoticed. (Pictures A and B, courtesy of Dr K. Jarjoura) Compare this result to a traditional autogenous gingival graft that is a lot more visible. (C) Adult who underwent 4 autogenous gum grafts (indicated by the arrows) to eliminate gum defects. The results of this type of procedure are less esthetic.
Connective tissue gingival grafts
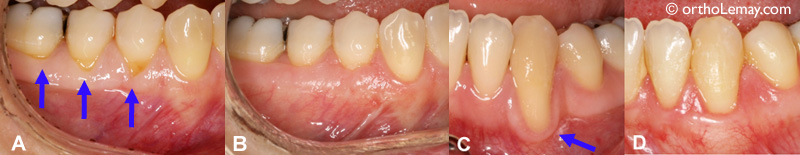
(A) Moderate gingival recession affecting posterior teeth. (B) 4 months after a connective tissue graft, the exposed roots are covered. (C) Severe recession affecting a lower canine. (D) 10 weeks after the surgical procedure. (Courtesy, Dr K. Jarjoura)
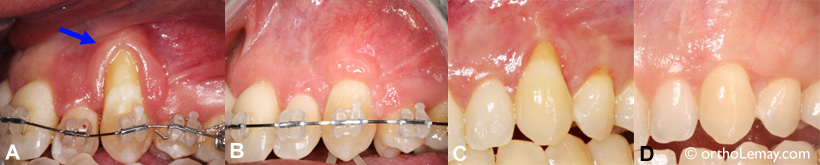
Receding gums affecting upper canines. (A) Severe gum recession that exposes a significant part of the root. (B) Following a correction with a gingival graft, the root is covered. (C) Moderate recession. (D) 3 months after the graft, esthetics is excellent. (Courtesy, Dr K. Jarjoura)
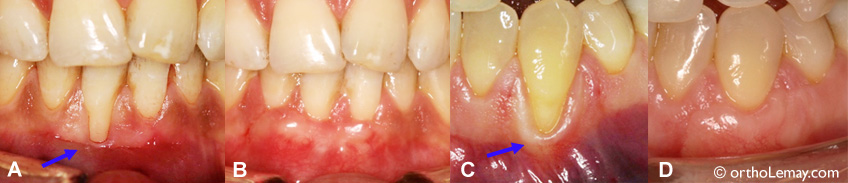
(A) Significant recession affecting a lower incisor. (B) A gingival graft made it possible to restore the normal gum level and cover the root (10 weeks after the graft). (C) Root of a canine that lost several millimeters of gum. (D) The graft tissue perfectly blends with the surrounding gum and protects the root. (Courtesy, Dr K. Jarjoura)
Autogenous gum grafts
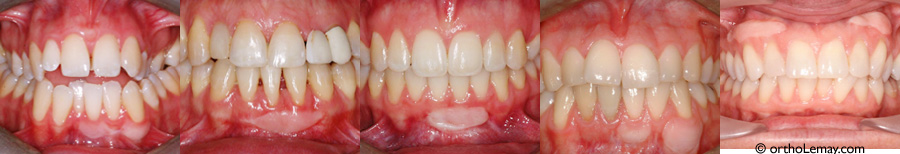
Autogenous grafts rarely provide results that are as esthetic as connective tissue grafts. There is no need to indicate where the grafts were performed on these pictures of different cases, they are very visible!
Recession on the lingual surface of teeth
Although it is less frequent, similar gum problems may also occur on the internal (lingual) face of teeth. Any tooth can be affected. The correction principles are the same as for a correction on the external face of teeth, but it is harder to perform for the practitioner and the patient, because it is more difficult to directly access the operative site and the tongue limits the space available in the lower arch.
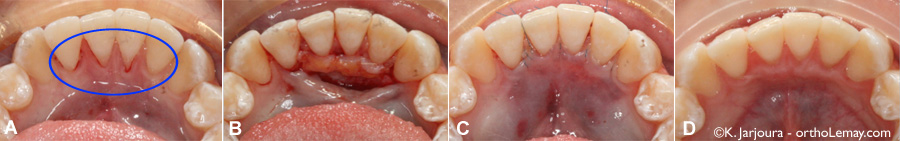
(A) Gum recession affecting the internal (lingual) face of the lower incisors. (B) During the periodontal surgery. (C) After the surgery with sutures in place. (D) Healing of the gingival graft after 4 months; the recession areas were covered. (Courtesy, Dr Karim Jarjoura)
Periodontics and malocclusions
- Preserving the supporting tissues of teeth (periodontium) is essential to the stability of the dentition and occlusion. Among others, this is what allows the teeth to keep a relatively stable position through time. Chronic periodontal diseases causing the loss of tissue weaken the support provided to teeth and this may influence the position of teeth indirectly.
- The forces applied to teeth by the perioral musculature (tongue, cheeks, lips) and masticatory muscles are normally well supported by an intact and healthy periodontium.
- However, when the periodontium weakens, these same “normal” forces may then progressively become too significant to be “supported” by a weakened periodontium. Then, tooth movement follows since the teeth give in to the various forces and pressures that act on them. Thus, we can see incisors that move forward and apart progressively throughout the years, creating new interdental spaces. Such a condition takes years or decades to develop and therefore, it is not present in teenagers or young adults, unless very particular problems occur.
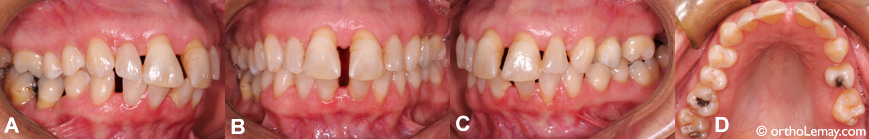
The loss of tooth support (bone and gum), coupled with the pressure of the tongue, can contribute to the creation of anterior spaces. (A to D) In this 49-year-old woman, the bone level supporting the teeth decreased throughout the years (periodontal problems). The teeth are not well supported anymore and they do not resist as much to the forces applied to them from normal function (chewing) and from the tongue that presses against the teeth. This may allow spaces to appear progressively even if this can take years or decades to occur.
To learn more on interdental spaces.
- In other situations, a malocclusion that is already present may contribute indirectly to periodontal problems. This is the case of Class II malocclusions with an excessive overbite and where the lower incisors “bite” into the palatal mucosa. Throughout the years, this condition causes recession behind the upper incisors and bone loss, which weakens the periodontium. The occlusal and chewing forces may then move the upper incisors forward, creating spaces and allowing the lower incisors to get longer and bite even more into the palate, thus generating a “vicious circle” that can lead to a severe destruction of the periodontium and even the loss of teeth after several years.
- The malocclusions that can cause such damages can be detected very early, as soon as infancy (see example below), and can be intercepted and corrected by an early orthodontic intervention. This is why it is recommended to perform a first orthodontic evaluation as early as 7 years of age.
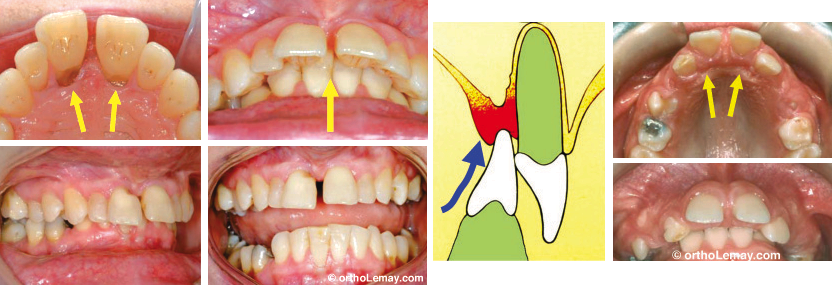
In the presence of an excessive anterior overbite, the lower teeth can bite into the palatal mucosa and damage it by causing recession and eventually, bone loss. A similar phenomenon, called posterior bite collapse, may occur when posterior teeth that serve as a “foundation” to the occlusion are lost. The loss of teeth causes anterior displacements, spaces, etc. To learn more on this subject, follow the link below.
➡ To learn more on posterior bite collapse.
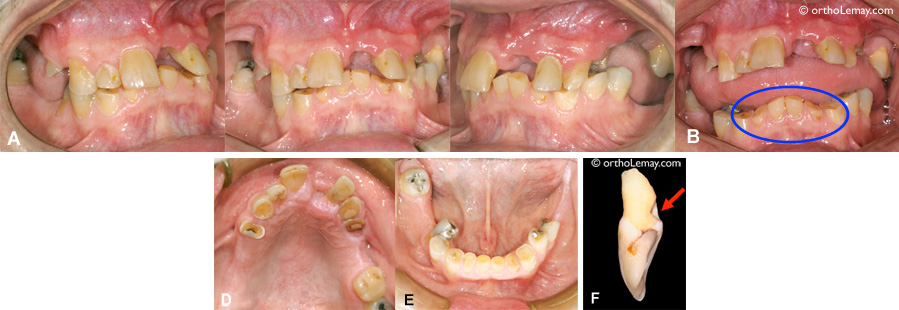
(A) This man, who is in his fifties, suffers from chronic bruxism. He is also affected by periodontal problems that caused the loss of a significant quantity of bone throughout the years. This, coupled with the excessive forces generated by bruxism, caused damages to his dentition and occlusion. The upper left incisor was so mobile that it fell off (see F). This tooth had a hole in it; it was caused by the lower tooth that always hit the tooth at the same place (arrow). (B) The lower incisors are 50-70% worn out. (D, E) No tooth is spared by this excessive wear, except the teeth that do not touch an opposing tooth.
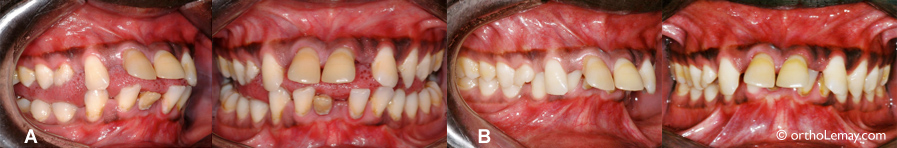
When the periodontium is weakened by the loss of supporting tissues, forces that are usually considered as “normal” may become too significant to be contained by the dentition. Therefore, in the case of this 24-year-old young adult, the periodontium of the anterior teeth suffers from a significant bone loss. The tongue that is already “hyperactive” in this mouth now constitutes a force that is too significant for the teeth to manage. Tooth movement then follows; the anterior teeth tip forward and move away from each other. (A) Usual “rest” position; the tongue applies a constant pressure to the teeth. (B) The way he bites when we ask him to move his tongue back voluntarily and “force” to close his teeth together. Note: The dark color of the gingiva is due to the fact that this person is black. The results of the orthodontic and periodontal treatment are illustrated below.
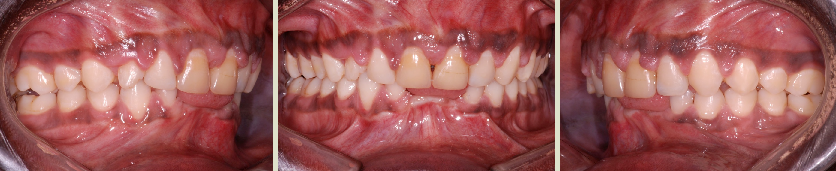
Despite the severity of the malocclusion and the periodontal problems affecting this young adult (24 years of age), an orthodontic treatment may be possible. This requires an interdisciplinary approach and a regular follow-up with a periodontist during the treatment. The very bad periodontal condition completely destroyed the bone surrounding the roots of the lower central incisors; these teeth could not be saved and had to be extracted. These pictures show the result after the orthodontic corrections.
Periodontal diseases
To understand periodontal diseases (gum diseases).
To learn more on gingival recession and bone loss.

 (27 votes, moyenne: 4.67 sur 5)
(27 votes, moyenne: 4.67 sur 5)


